As published in Columbia Journalism
“Don’t Let Them Die Alone”
Ariana Baio
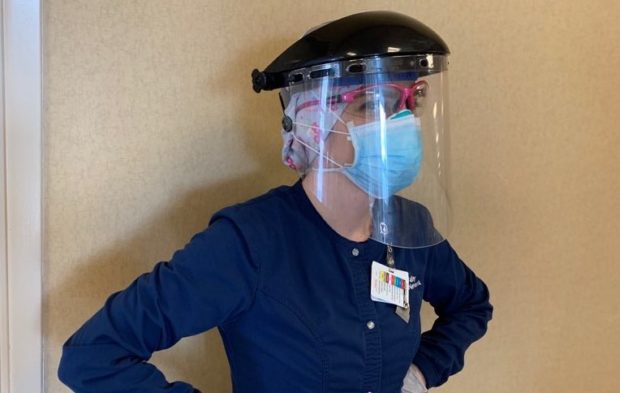
Ashley Chuhran has spent seven years as an intensive care unit nurse caring for patients on the brink of death. Not much scares her.
But sweating profusely underneath a gown, scrubs, two pairs of gloves, a hairnet, two masks and a face shield, She feared for her life while trying to save one of her first severely ill patients in March 2020. For several days the patient, a man in this ’60s, seemed to be getting better. Then, suddenly, his vitals dropped.
The other ICU nurses and Chuhran, 37, tried to make sense of the situation. They often spoke with the man’s family and surrounded him with the photos and handmade cards the family sent. It had been over 40 days since he was admitted into the ICU. They tried everything to help the man but there were still other patients who needed attending to.
Chuhran remembers the horror of the early, hectic days. Of the 32 patients in her ICU, she said, 10 were proned–a rarely used face-down position patients in respiratory emergencies are laid to avoid the use of a ventilator.
“I’m walking down the hallway and all thesepatients prone and I’m like, ‘Oh my god, we’re all going to die,’” Chuhran said.
Like many other nurses, Chuhran provided a lot more than medical care for COVID-19 patients. She was often a vital link between the patients and their families. She brought cards, gifts and words of comfort. Sometimes she was the last person that a dying patient would see.
It was the early day of the pandemic and already all 32 beds in Pennsylvania’s Lehigh-Valley Cedar Crest ICU were occupied with patients suffering from the virus.
“I went into nursing to be able to be with my patients and get to know them and take care of them like I would take care of my family, but a lot of the time I can’t do that,” Chuhran said.
Caring for others was ingrained in Chuhran from a young age. She grew up in Reading, Pa. in a close-knit family: mother, father and older brother.
She often bore witness to her immediate and extended family’s caring nature. Her dad, who had hepatitis C most of his life, sometimes required extra care from her family during periods of medical complications. She watched her aunt take care of her grandfather while he was sick too. So, when it was time for Chuhran to pick a first “real” job, she knew she wanted to help people.
At 19, she started working at an assisted living facility and became a certified nurse assistant, helping pass out medications to elderly residents.
Working at the assisted living facility gave Chuhran her first experience with a dying patient. She developed a bond with a woman ready to die who had no family left to be with her. Chuhran had never seen anyone die before.
“I knew that I needed to be with her.” Chuhran remembered, “so I just sat there with her and it wasn’t as dramatic as I thought it was going to be. It was very quiet, just really peaceful.”
This became a lesson Chuhran has carried throughout her nursing career: to be there with a dying patient, regardless of circumstances.
“I think it’s a blessing to be there with them when they’re dying,” she said.
Working at the assisted living facility allowed Chuhran to tap into her sympathetic nature, but she knew that she could not survive on the salary she was getting as a nurse assistant. A career in nursing was humming in the back of her mind.
But it was her father’s death that pushed her to accelerate her career.
Chuhran watched her father struggle through years of complications. A year prior to his death, he needed a liver transplant which left him on transplant medications. After a series of problems with his blood pressure, he had a massive stroke which left him with a brain hemorrhage. Ultimately, he was put on life support, and Chuhran and her family painfully made the difficult decision to take him off life support.
“I think there’s a big misunderstanding between making people comfortable and trying to keep them alive,” Chuhran said. “Does this family want their family to be in a nursing home on a trach with a ventilator? They don’t see the long road ahead, and these patients end up dying anyway.”
At 24, Chuhran began pursuing a bachelor’s in nursing at Alvernia University in Reading, Pa. Nursing school did not come easily to her, though. She described the experience as “wanting to light myself on fire.”
As difficult as it was, school also introduced Chuhran to her best friend, Julie Fisher, who is now an integral part of her support system.
“We really complement each other,” Fisher, 34, said. Where Fisher is reserved, Chuhran is outgoing.
The two quickly formed a bond in school and helped each other study for tests and prepare for their future careers in nursing. Even after graduating, Fisher and Chuhran carpooled to work together. Their friendship has remained through work, marriage, kids and everything in-between.
“It’s nice to have someone to talk to that understands and knows what it’s like,” Fisher, who is a nurse at Lehigh-Valley Cedar Crest, said. “It’s easy to come home and talk to your spouse about it, but they don’t really get the day-to-day stressors we actually go through.”

Chuhran graduated from Alvernia at 28 and walked into Lehigh Valley Cedar Crest Hospital in Allentown ready to take on any patient thrown her way. She started on the medical-surgical floor–the area designated for patients who do not need critical care–otherwise known as med-surg.
“I didn’t enjoy that because it’s a really high turnover rate.” Chuhran said, “There was not a lot of time to focus on your patient and take care of your patient.”
The one-on-one time that Chuhran had while working in the assisted living facility was the type of care she was looking to provide, and med-surg was not fulfilling that need.
Forming a relationship with a patient, understanding them and providing the care they need is extremely important to Chuhran. Her entire nursing career is based on her desire to help patients through knowing them rather than just reading a chart for a few seconds and making a decision.
“Her best quality is getting people to open up and make them feel comfortable,” Fisher says. “She makes you feel like she wants to be there with you and listen to you.”
Chuhran’s strength in nursing was best fit where many will not go, the ICU. She thrives in the fast paced environment where she can connect with patients one-on-one. But the pandemic has tested this.
During the first wave of the pandemic, Chuhran’s hospital stopped elective surgeries and asked extra staff to assist the ICU. The hospital was caring for around 230 COVID patients in April 2020, nearly a third of the facility’s 729-bed capacity, and needed all the hands they could get. But closing elective surgeries meant the hospital was losing revenue, so when the opportunity to resume them emerged, they did. This left the ICU short-staffed during the second wave.
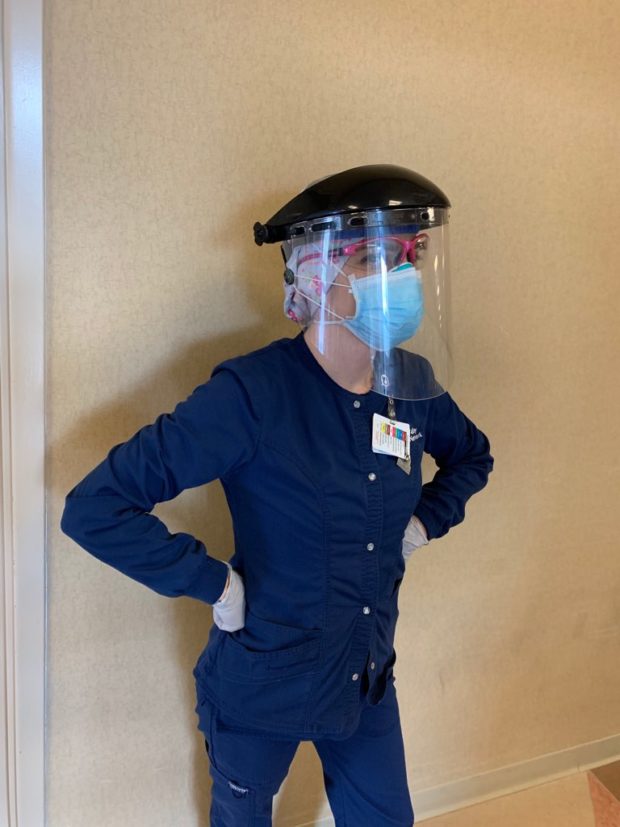
The second wave of COVID hit Lehigh Valley Cedar Crest significantly worse. At its peak, the hospital had around 530 patients in January 2021 with only 16–18 ICU nurses available on rotation. Chuhran was getting tripled, meaning she was forced to care for three patients in critical condition rather than the typical one.
Nursing shortages are a problem without a pandemic, but the effects of short staff were heightened during COVID. Chuhran was working 12-hour shifts in heavy personal protective equipment, often without a break to eat or use the bathroom. Trying to assist patients in their physical needs while supporting them mentally and emotionally was exhausting.
“The things she sees at the ICU are hard to separate and leave at work,” Fisher said.
Chuhran has borne witness to the suffering the pandemic has caused. She has sacrificed her time, energy and mental wellness to attend to others’ needs. It was a difficult journey becoming an ICU nurse, but Chuhran was sure of her desire to care for people. She was confident in her ability to let patients die in a comfortable and safe space. But watching patients die in the same way as her dad, being taken off life support by families has made her question her career.
“Plenty of times I wanted to leave,” Chuhran said. But, inevitably, she stays. “I don’t know what else I would do; I couldn’t do anything else.”
The man in his 60’s who Chuhran cared for was ultimately taken off life support by his family. He died shortly after. But like most of Chuhran’s patients before, he did not die alone. Nurses stood by him, ensuring he received the grace he deserved, despite the chaos. Chuhran and the other ICU nurses continue to do so.
